Introduction to Diagnostic Medical Parasitology
Essentials
The infectious agent of American trypanosomiasis, Chagas disease, is the haemoflagellate Trypanosoma cruzi. Infection of humans occurs by contamination with freshly infected bug faeces of blood-sucking species of Reduviidae (kissing bugs) or by the bite of an infected bug: - Conjunctivae - Mucous membranes - Skin wounds
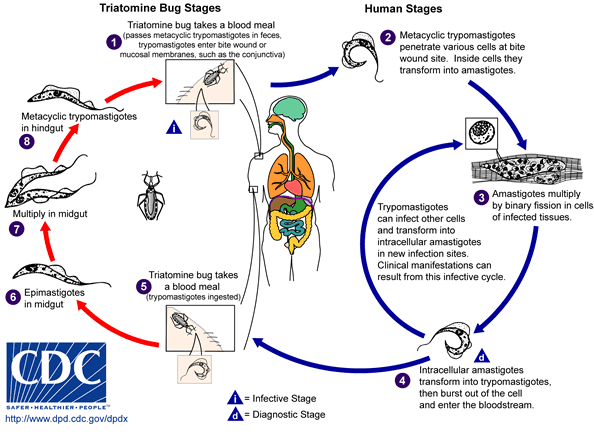
T. cruzi undergoes morphogenesis during its life cycle. The trypomastigote and some intermediate forms with a flagellum are found in the peripheral blood. They invade host cells (cardiac and striated muscle fibres) and change to the amastigote form with a truncated flagellum. The bugs become infected when they feed by biting on a parasitaemic human or animal. In the insect gut, the trypomastigotes change to promastigotes which multiply, change to infectious metacyclic trypomastigotes in the rectum and are then excreted with the faeces.
Epidemiology
- Chagas disease is found in rural areas of Latin American countries due to sociocultural factors (housing, poverty, hygiene)
- The kissing bugs (Triatoma sp.) become infected when they feed on a parasitaemic human or animal
- Infection of humans is by bite of infected bugs or via blood transfusion
- Reservoirs are humans and over 150 species of domestic and wild animals (they can become infected by ingestion of infected bugs!)

Pathology
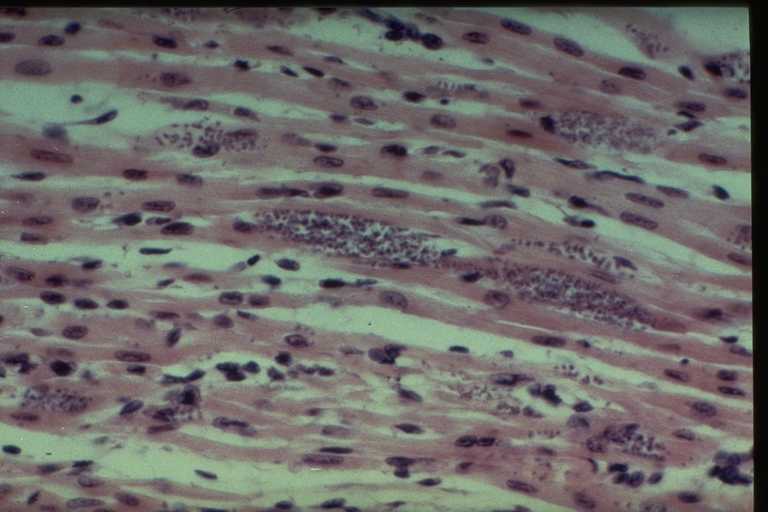
- Acute phase: after local invasion of histiocytes and draining lymph nodes, trypanosomes are disseminated via the blood stream. Destruction of host cells by multiplying amastigotes leads to inflammation, oedema and fever. Enlargement of liver and spleen.
- Chronic phase: either asymptomatic or cardiac and CNS manifestations
Clinical Findings
- Incubation period:
5–14 days after the bite of the bug
30–40 days following transfusion of infected blood - Acute disease generally in children, while irreversible chronic manifestations appear later in life
- Acute disease: fever, malaise, lymphadenopathy and hepatosplenomegaly. Fatal complications include myocarditis and meningoencephalitis.
- Chronic irreversible sequelae: myocardial damage: cardial dilatation, arrhythmias, conduction abnormalities; gastrointestinal damage: megaoesophagus, megacolon
Diagnosis
Diagnostic methods
Parasitological diagnosis
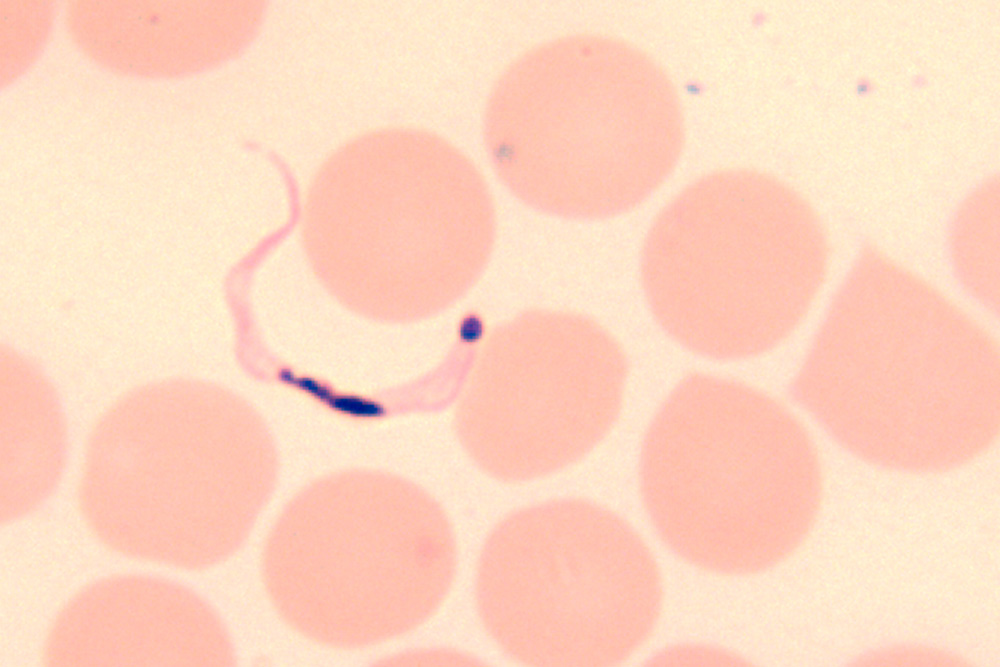
The definitive diagnosis of American trypanosomiasis (Chagas disease) is done by detecting trypomastigotes in the blood after concentration.
Parasitaemia is highest during acute febrile episodes early in the course of the disease. Parasites are rarely detected in lymph nodes or skeletal muscle.
In chronic often asymptomatic infections, no trypanosomes can be found in the peripheral blood due to immune elimination.
Molecular diagnosis
Detection of DNA in the blood or in tissue samples is a new alternative to confirm serological screening results. Nested and real-time PCR methods have been developed to detect Chagas infections in the blood or in biopsies.
Antigen detection
No tests are available
Antibody detection
Serological methods are important for the screening of exposed populations. A series of serological tests have been commercialized using different test formats (mainly IFA and ELISA).
Diagnostic strategies
- To diagnose an individual case
In acute infections, the parasite might be detected in the blood. If this is not achieved, serology or molecular diagnostic methods could be used.
Due to these newer methods, xenodiagnosis, i.e. to see whether reduviid bugs become infected after taking a blood meal on the patient – has become obsolete.
- To assess endemicity in an endemic area
The optimal method would be to use rt-PCR if available.
Prevention and control
- Education of people in endemic areas about the risk from “kissing bugs”
- Systematic eradication of the bugs in the houses by spraying residual insecticides
- Improved housing which reduces the number of bugs
- Screening of blood or organ donors from endemic areas