Introduction to Diagnostic Medical Parasitology
Leishmaniasis, mucosal
Essentials
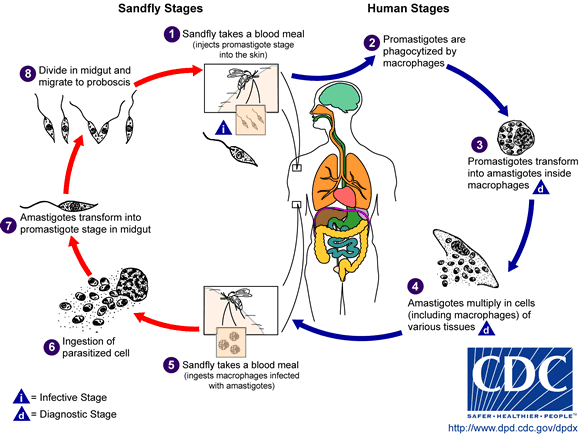
Leishmaniae are protozoa belonging to the family Trypanosomatidae. On clinical grounds, they have been divided into three major groups: cutaneous, mucocutaneous and visceral. They consist of many different species and subspecies. The New World mucocutaneous leishmaniasis species are within the L. mexicana and L. braziliensis complex representing many different species.
Epidemiology
- Distribution in endemic foci from southern Texas to northern Argentina
- Exposure is by activities in lowland forests
- Many wild animals are natural hosts (sylvatic zoonosis); domestic dogs can also become infected
Pathology
- Skin ulcers with chronic inflammation, pseudoepitheliomatous hyperplasia and granulomatous inflammation
- Mucocutaneous leishmaniasis causes facial disfigurement
Clinical Findings
- The incubation period lasts from 2 weeks up to many months
- Primary cutaneous lesions (mainly ulcers) are painless
- Mucosal involvement after a primary cutaneous lesion
- Espundia occurs in an ulcerative and non-ulcerative form
- Complications arise through secondary bacterial infections
Diagnosis
Diagnostic methods
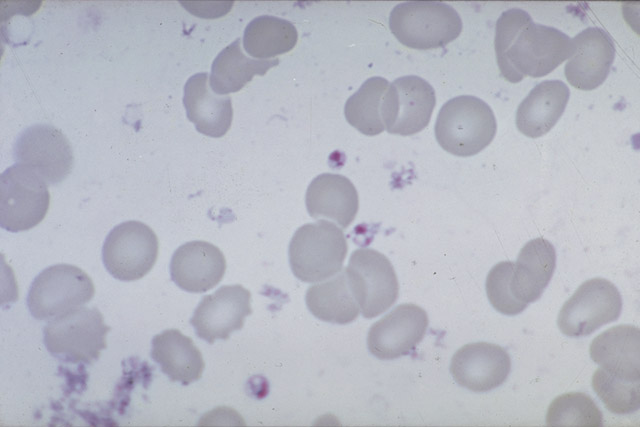
Parasitological diagnosis
Mucosal leishmaniasis is an important complication of South American cutaneous leishmaniasis.
Diagnosis is made by demonstration of the parasite in affected tissues. In the past, tissue samples were put into special cultures to demonstrate multiplication of promastigotes. Today, PCR offers a more sensitive and rapid alternative.
In rural areas, the Montenegro skin test is still in use. This test has a good sensitivity but cannot discriminate between acute and past infections.
None of the parasitological tests is considered a gold standard anymore.
Molecular diagnosis
Highly sensitive and specific nested and real-time PCR methods have been developed to detect DNA in mucosal samples. PCR is also possible with formalin-fixed histological samples!
Antigen detection
No tests developed so far
Antibody detection
Circulating antibodies can be detected in many but not all cases of mucosal leishmaniasis. The specificity of serological methods is rather low.
Diagnostic strategies
In endemic areas, diagnosis is often done on clinical findings. Definite diagnosis can only be reached with molecular methods.
Prevention and control
- Protection against bites by infected sandflies (clothing and repellents)
- Use of fine-meshed mosquito nets